PHOTO
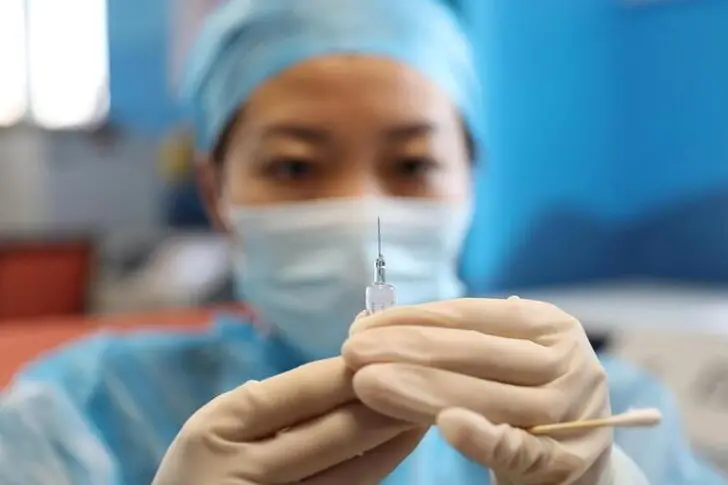
Less than a year after the world was first hit by the coronavirus disease (COVID-19) outbreak — which has gone on to become the worst pandemic in more than 100 years, killing almost 2 million people so far — the world already had its first vaccines.
Within weeks of China first reporting the virus, the leaders of the developed world, notably the US and Europe but also China and Russia, threw their weight behind the development of vaccines that could counter the pandemic.
Thus, by April last year, a race of sorts had begun between leading pharmaceutical firms such as Pfizer and Moderna in the US and AstraZeneca in the UK to develop a vaccine. The race was ignited and funded — generously one ought to say — by governments, with both UK Prime Minister Boris Johnson and US President Donald Trump opening up their countries’ treasure chests to help the companies.
The US government paid both Pfizer and Moderna about $2 billion each for the advance purchase of 100 million doses of their vaccines — a significant incentive for the two firms to dive head-long into the superfast development of a vaccine. In the EU, a clutch of nations also made advance purchases, ensuring that the pharmaceutical firms ran no risk on their investments and instead were assured of huge rewards upon the successful development of a vaccine.
Within months, the pharma companies had scaled up plans to manufacture vaccine doses by the end of the year, with an average production target of more than 200 million doses in 2020 and more than a billion in 2021. Flush with funds, the firms lost no time in conducting research and, soon enough, more than 200 potential vaccines had been identified. Progress moved at an electric pace toward clinical and subsequently human trials.
This was by far the fastest rollout of any drug ever. Some of the credit for the pace must also go to the drug regulators around the world, who played their role by clearing the proposals and cooperating with the pharma firms, instead of their normal adversarial relationship. The regulators offered fast-track approvals at all stages, including the final emergency use authorizations that have now been issued by health regulators in many countries.
This collective approach and the fast-tracking of the vaccines, as well as the serious nature of the pandemic, have seen many countries launch their own vaccine development projects. According to GAVI, the Vaccine Alliance, at least 154 vaccines are being explored in lab experiments, while 20 others are undergoing Phase 1 trials, 16 are in Phase 2, and 13 in Phase 3. This is no mean feat, considering that all this was achieved in less than a year and against a virus of which humanity had no previous knowledge.
One of the brightest spots in the COVID-19 vaccine development is a unique project led by the World Health Organization (WHO) that aims to ensure the availability of affordable vaccine doses for poorer countries. The WHO project has been funded by a clutch of rich and middle-income countries and several other donors, who have raised billions of dollars in a short period of time. This has enabled the project to not only get off the ground, but also make serious progress with the aim of rolling out vaccine doses at highly competitive prices or even for free, depending on the recipient countries and their means.
The various initiatives taken up by the global community, together as well as unilaterally, are highly encouraging and positive for global health. But it will not be enough to restrict this to merely tackling the COVID-19 pandemic. It is important for world leaders and pharmaceutical companies to realize that the way in which they have gone about coming up with plausible solutions to tackling this new virus at a rapid pace should be replicated to attack many other illnesses that have been the bane of humanity for centuries or more. Every such disease is highly contagious and causes billions of dollars of economic losses each year as well as being deadly, with millions of victims. The casualties of each of these diseases — whether they are global like malaria and tuberculosis or more limited like Ebola — need to be treated with the same degree of urgency and commitment for two reasons.
Firstly, over the decades and even centuries of prevalence of these illnesses, humanity has built up a lot of experience of them, their symptoms and how to treat them. This should make the development of vaccines much easier than in the fight against COVID-19.
The other reason is that most of the countries afflicted by these diseases are extremely poor, with little healthcare infrastructure, pharmaceutical industry or budgets to battle against the illnesses. They need the global community, notably Big Pharma and the governments of rich countries, to be able to take on these diseases.
The global alliance against COVID-19 is a very clear illustration of how humanity can join hands and overcome such challenges. It is now time for all these stakeholders to continue their cooperation and jointly develop vaccines against more diseases. It would be a pity if the world let go of the sense of brotherhood and the momentum that has been built up. Ultimately, the costs would be a fraction of what the rich nations have used in fighting the pandemic, while Big Pharma may want to use some of its huge gains from the COVID-19 vaccine windfall — money that has come from the pockets of people all over the world — for the development of other vaccines.
- Ranvir S. Nayar is managing editor of Media India Group.
Copyright: Arab News © 2021 All rights reserved. Provided by SyndiGate Media Inc. (Syndigate.info).